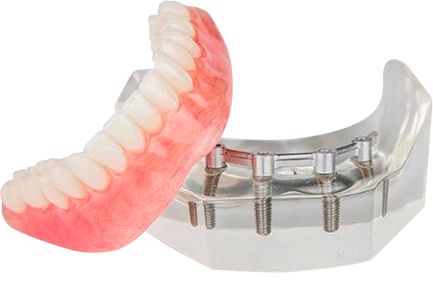
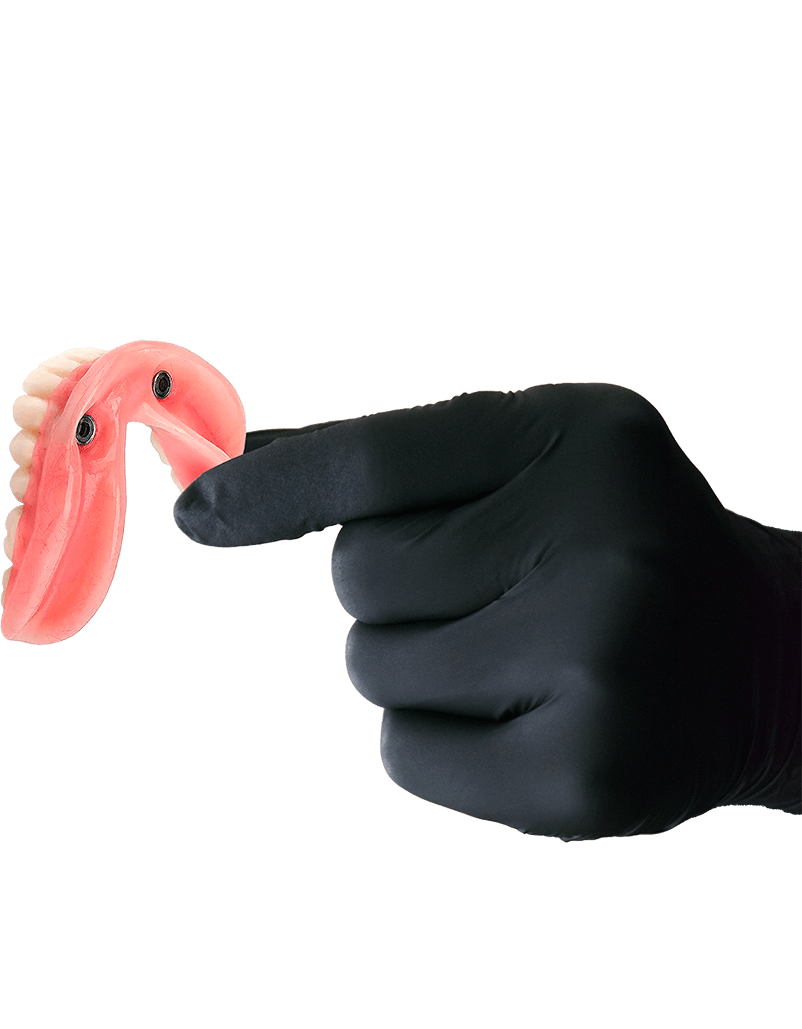
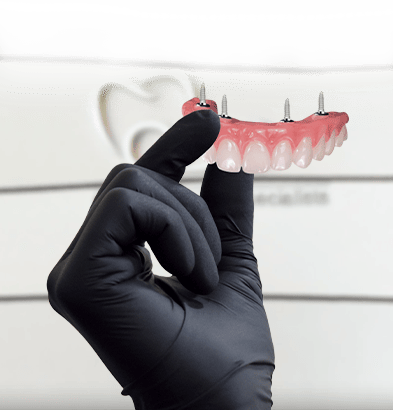
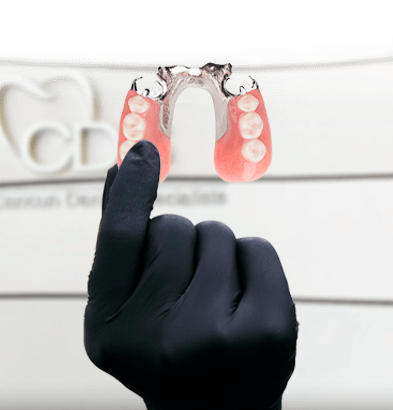
THINGS TO CONSIDER BEFORE GETTING SNAP-ON DENTURES IN MEXICO
We understand that visiting a dentist in another country creates different concerns for you, as many of our patients have told us:
- Who will perform my treatment?
- What dental technology do they use?
- How much are snap-on dentures in Mexico?
From our experience of more than 20 years, we can say that everyone who has visited us at Ocean Dental Cancun, leaves fascinated. Both with the service and the dentists, not to mention the prices that can save you thousands of dollars compared to the US.
OVER 5K PATIENTS COME FOR SNAP-ON DENTURES IN MEXICO YEARLY
- About 23 million are completely edentulous.
- About 12 million are edentulous in one arch.
90% of those
who suffer from edentulism have dentures
ARE SNAP-ON DENTURES IN MEXICO REALLY THAT GOOD?
Same Quality as in the US?
In addition to having affordable snap-on dentures prices, the quality of Mexico’s dental work has been improving its recognition all over the world.
And so does Ocean Dental Cancun, where you can find the best trained dentists, top technology and professional service.
What Problems Can Be Solved With Snap on Dentures?
There are some dental conditions that make snap on dentures the right solution for you.
- Decreasing Jaw Bone Density
- Chipped or Fractured Teeth
- Multiple Missing Teeth
- Being Edentulous
- Use Traditional Dentures
- Need Decayed Teeth Extraction
In addition to the problems clip on dentures can solve, they also have other advantages when used such as:
Better Support than Traditional Dentures
As snap on overdentures are supported by dental implants, they provide additional strength to the jaw bone and a more balanced stability. Which comes to better retention with no risk of falling off.
Palateless Implant Dentures
Unlike traditional dentures, implant supported dentures are completely palateless, meaning they do not have the commonly uncomfortable roof of the mouth. Leading to a better sense of taste when eating.
Great Comfort & Aesthetics
Another important benefit for snap on dentures is the comfort provided feeling like natural teeth. And the aesthetics they have, being made of acrylic but looking completely natural. Giving you a perfect smile!
COST OF SNAP ON DENTURES IN MEXICO
Many patients turn to Mexico for their treatment because of the affordable snap on denture prices, where the cost at Ocean Dental Cancun starts at $4,200 USD for Snap-on MDi (Mini Dental Implants) and $6,760 USD for Snap-On RDi (Regular Dental Implants).
Snap on – RDi
No More Dentures
Starting At
$6,760 USD
4 Regular Dental Implants Final Acrylic Prosthesis
Snap on – MDi
Minimally Invasive
Starting At
$4,200 USD
6 Mini Dental Implants
Final Acrylic Prosthesis
BENEFITS OF GETTING SNAP-ON DENTURES IN CANCUN
Aside from the low cost of dentures, getting your snap on dentures in Mexico brings with it various advantages such as excellent dental work, the best quality for each treatment, and dental vacations among others:
Implant Dentistry Experts
Ocean Dental Cancun is internationally recognized as a dental clinic expert in implants, with the best reviews in Mexico.
Specialized Prosthodontists
Every prosthesis used for an implant restoration is done and delivered by our prosthodontists, specialists in elaborating full arch bridges.
Shorter Dental Work Timeframes
The focus we have with dentistry procedure is to deliver every treatment with excellence, quality and in the shorter time possible, so you can return to your country with smile that you came for in 7 to 10 days on average.
Custom-Made for Your Smile
With our innovative technology smile design software, we can personalize the way your new smile will look, to your preference.
Long-Lasting Results
Thanks to the materials we use, as acrylic for the prosthesis and titanium for implants (mostly) we can, we can assure you long lasting results. A new smile for a lifetime.
Ease of Travel
As Mexico is next to the United States and the closest dental destination for Canada, there will be no other place that provides the ease of travel as Mexico.
Dental Vacation in Cancun
Enjoy of the beautiful beaches in the Mexican Caribbean, staying at five star resorts and exploring what Cancun has to offer, all this while treating your teeth for a better and healthier smile.
Little Recovery Time
Whether it be done with regular dental implants or mini dental implants, we can assure you the recovery time will not be of a year or more, as it commonly is in the US or Canada.
HOW LONG DOES IT TAKES TO GET SNAP-ON DENTURES IN MEXICO?
By coming to Ocean Dental Cancun you can get your snap-on dentures in only 10 days (this could change depending on your condition), thanks to the use of the latest and less invasive type of implants: mini dental implants.
How Much Do Snap-On Dentures Last?
With proper care, snap-in dentures can last more than 10 years. Of course, you should consider replacing abutments every year, and regular check-ups with your dentist to verify any possible complications or changes during the lifetime of your implant-supported denture.
SNAP ON DENTURES IN MEXICO REVIEWS
SNAP ON DENTURES VS OTHER TREATMENTS
Snap on Dentures
vs All on 4
Speaking of aesthetics, as much as snap on dentures imitate your natural teeth color, all on 4 gives a better look because of its multiple material options.
Finally going through the prices, you can see snap on dentures are much more affordable, thanks to its way of usage and the acrylic material used to elaborate the prosthesis.
Snap on Dentures
vs Partial Dentures
Partial dentures can be fitted when you have remaining healthy teeth, to avoid the need of extraction.
Although, they cannot be held by dental implants. So, we recommend our patients to use snap on dentures, because of its comfort, security, and confidence provided when eating, laughing or smiling.
Snap on Dentures
vs Fixed Dental Bridges
Dental bridges are used to cover your missing tooth spaces with a permanent restoration. But can’t be used when you have various missing teeth.
That’s when full arch implant restorations enter, although some of our patients can’t afford an all on 4 or 3 on 6, we always recommend snap on dentures because of its versatility.
SNAP-ON DENTURES WITH MINI DENTAL IMPLANTS
The Least Invasive Alternative for Dental Implants
Mini dental implants do not require deep surgery for implant placement causing less trauma to the jaw bone. In addition, they allow receiving the permanent snap-on denture immediately after implant placement, which can be considered as your teeth in a day.
WHAT IS THE PROCESS TO GET MY SNAP-ON DENTURES IN CANCUN?
For regular dental implants you will need to make two trips: the first one for the implant placement and the temporary prosthesis. And, the second one will occur from 4 to 6 months, after the healing and osseointegration phases, to place the permanent snap on denture.
As for mini dental implants, as mentioned before, they only require one trip of 10 days on average to place the implants and the final restoration.
1st Visit
Pre-Oral Evaluation
First, at the moment of your arrival, our private transportation will pick you up and take you to the clinic so we can start elaborating your treatment plan and begin with your initial consultation.
Additional Treatments
After it, the next day or the same day (depending on your disposal) we will undergo the additional treatments needed as a bone graft or root canals, so there is no failure range for the implant surgery.
Implant Placement
On approximately the fourth day of your stay, we will begin with the implant placement with requires sedation and surgical guides (Navident technologies).
This will be fully attended and delivered by our expert implantologists and prosthodontists.
Teeth in a Day
This phase is where the difference between alternatives enters:
For the regular dental implants, you will need to wear the temporary prosthesis for about 4 to 6 months. While for mini dental implants, in this phase you will receive your permanent restoration.
2nd Visit
Healing Evaluation
Continuing with regular dental implants, after the healing period is over.
On your second trip, the first consultation will be to see how the process has been going, if there has been any complication or if you have any uncertainties as well.
Permanent Restoration
Following the consultation, we will begin removing your temporary prosthesis so it is possible to place the permanent snap on dentures made of diamond acrylic.
Post-Assessment
After it, we will keep monitoring the progress, if it needs any adjustments and if not, be ready to smile like never before!
SO, SHOULD I GET SNAP-ON DENTURES IN CANCUN
Getting snap-on dentures is an excellent alternative to restore your smile without paying higher prices for all-on-4 or 3 on 6.
As well it is important to say snap-on dentures gives you both, cosmetic and functional benefits such as recovering your teeth by feeling comfortable and having a good natural-looking smile.
So, yes! In short term, you should get snap-on dentures in Mexico to have the comfort of smiling as you would like to, anytime, anywhere, with the people around you.
You can get started by sending us a message or calling us directly, so we can help you plan your trip to Cancun to get your dental crowns.